Analgesic or pain medicines are the most commonly prescribed medicines. Analgesic misuse is common because the patient needs quick relief and the doctor needs quick results.
The most commonly used pain medicines include:
Apart from paracetamol, codeine, and
tramadol which have little anti-inflammatory effects, most of the other drugs reduce inflammation (NSAIDs).
Reduction in inflammation and improvement in the symptoms of pain results in masking of some serious underlying disorders.
I am presenting here a case highlighting the importance of diagnosis. Physicians must strive to diagnose the patient first and then write pain medicines if required.
How Analgesic Misuse resulted in a delayed diagnosis!
A middle-aged lady presented with pain and swelling of the left knee joint for the past three years.
She started having mild to moderate pain along with swelling of the left knee joint 3 years back which worsened with movements.
It was associated with a low-grade fever and early morning stiffness for about 30 minutes.
There was no history suggestive of pain in any other joint, oral ulcers, hair loss, or other systemic symptoms.
She visited multiple physicians and orthopedic surgeons. She was advised blood tests including RA factor for
Rheumatoid arthritis and uric acid for gout but every time the reports were normal.
She remained on the following analgesic medicines during these three years:
Apart from the above medicines, she was also prescribed turmeric tablets that contain curcumin.
Turmeric is a natural product used as a spice in Asia (India, Pakistan, and China). It acts by inhibiting the selective COX-2 enzyme just like celecoxib and etoricoxib resulting in anti-inflammatory properties.
Turmeric supplements are nowadays commonly prescribed for rheumatoid and osteoarthritis especially by orthopedic surgeons and are thought to have anti-inflammatory and immunomodulatory properties.
Her symptoms would improve partially and temporarily.
One week back she visited our clinic. She was limping and was brought with the help of support by the family members.
On examination, she had a swollen left knee joint with effusion, warmth, and restricted mobility.
The rest of the systemic examination was unremarkable.
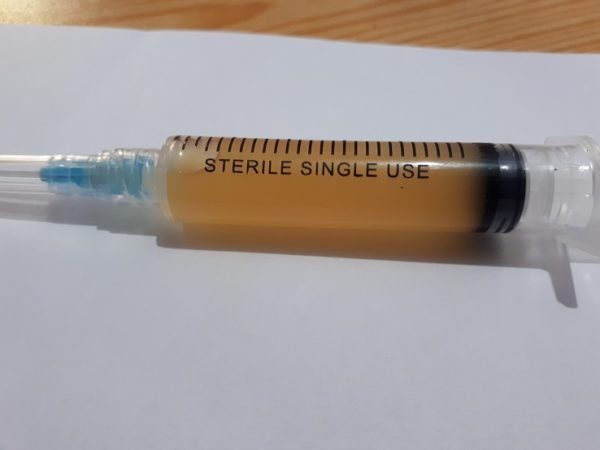
I proceeded for a synovial fluid aspirate.

You can see here that the fluid is very turbid and dirty yellow in color.
The synovial fluid was sent for a routine examination, gram stain, AFB smear, bacterial and AFB culture, and Gene Expert (PCR for Rifampicin resistance).
The prolonged history, low-grade undocumented fever, and the septic joint with turbid synovial fluid tempted me to start anti-tuberculous therapy without even waiting for the results.
She was started on:
The results of the synovial fluid analysis were confusing ...
- The test was negative for any bacteria or mycobacterium tuberculosis.
- WBCs in the synovial fluid: 760 cells/mm³
- Proteins: 2.3 gms
- Glucose: 97 mg/dl
The final words:
Physicians must try to identify the underlying cause of pain or inflammation. Analgesic misuse may mask the symptoms of underlying serious conditions as in the case presented here.
What should I do next?
-
Should I continue the anti-tuberculous therapy, keeping in mind the long history of monoarthritis and a turbid synovial fluid?
-
Should I repeat the test from a better lab?
-
Should I just see the clinical response to therapy?
-
Or any other suggestion? ( The patient belongs to a poor socioeconomic state).
 You can see here that the fluid is very turbid and dirty yellow in color.
The synovial fluid was sent for a routine examination, gram stain, AFB smear, bacterial and AFB culture, and Gene Expert (PCR for Rifampicin resistance).
The prolonged history, low-grade undocumented fever, and the septic joint with turbid synovial fluid tempted me to start anti-tuberculous therapy without even waiting for the results.
She was started on:
You can see here that the fluid is very turbid and dirty yellow in color.
The synovial fluid was sent for a routine examination, gram stain, AFB smear, bacterial and AFB culture, and Gene Expert (PCR for Rifampicin resistance).
The prolonged history, low-grade undocumented fever, and the septic joint with turbid synovial fluid tempted me to start anti-tuberculous therapy without even waiting for the results.
She was started on: